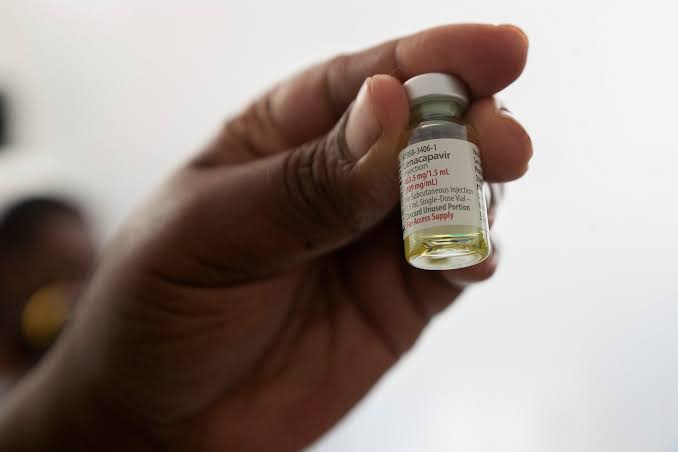
Uganda’s introduction of lenacapavir, a breakthrough HIV prevention drug, signals more than just the arrival of a new medicine. Health experts say it represents a fundamental shift in how HIV can be prevented, particularly among high-risk populations.
The long-acting injectable, developed by Gilead Sciences and delivered through a partnership between the United States and the Global Fund, is being rolled out under the leadership of the Ministry of Health.
A different way of stopping HIVUnlike traditional HIV prevention pills that must be taken daily, lenacapavir works by targeting a critical stage in the HIV life cycle. It blocks the virus from replicating inside the body by interfering with the protective “capsid” shell that HIV needs to survive and multiply.
By disrupting this process early, the drug prevents the virus from establishing infection in the body—even if exposure occurs.
Medical researchers describe this as a major scientific advancement because it attacks HIV in a way that is different from most existing prevention drugs, offering a powerful new line of defence.
Twice-a-year protection
One of lenacapavir’s most distinctive features is how it is administered. Instead of daily pills, the drug is given as an injection just twice a year, roughly every six months.
This long-acting formulation allows the medicine to remain in the body at protective levels over an extended period, steadily working to block infection without the need for frequent dosing.
For many users, especially those who struggle to maintain daily medication routines, this could significantly improve adherence and overall protection.
“It removes the burden of remembering to take a pill every day,” a health official involved in the rollout explained. “That alone can make a huge difference in real-world effectiveness.”
Simple but structured delivery
The administration of lenacapavir follows a structured clinical process. Individuals first undergo HIV testing to confirm they are HIV-negative before receiving the injection.
Once cleared, the injection is administered by trained health workers, typically in a clinical setting. Follow-up visits are scheduled every six months for the next dose, along with routine monitoring and support.
Health officials say the simplicity of this schedule makes it easier to integrate into existing health services, including maternal care and youth-friendly clinics.
Why it matters for Uganda
Uganda continues to record nearly 37,000 new HIV infections annually, with adolescent girls, young women, and mothers among the most affected groups.
Experts believe lenacapavir could be particularly effective in these populations, offering discreet, long-term protection without the stigma or logistical challenges associated with daily medication.
Its high efficacy, over 99 percent in clinical trials, means it has the potential to dramatically reduce new infections if widely adopted.
Expanding access
Under the current rollout plan, Uganda is expected to receive enough doses to cover about 46,000 people in 2026, with expansion planned in subsequent years.
The broader global initiative aims to reach up to 3 million people by 2028, with Gilead Sciences supplying the drug at cost and supporting the production of more affordable generic versions.
Not a standalone solution
Despite its promise, health experts caution that lenacapavir is not a replacement for other HIV prevention strategies.
Testing, education, condom use, and treatment programmes remain essential components of the overall response. Instead, the new drug is expected to complement these efforts, adding a powerful tool to the prevention toolkit.
A shift in prevention strategy
As Uganda begins rolling out lenacapavir, the focus will be on ensuring access, awareness and consistent follow-up care.If successfully implemented, the twice-yearly injection could redefine HIV prevention, making it simpler, more effective and more accessible, and bring Uganda closer to its goal of ending HIV as a public health threat by 2030.